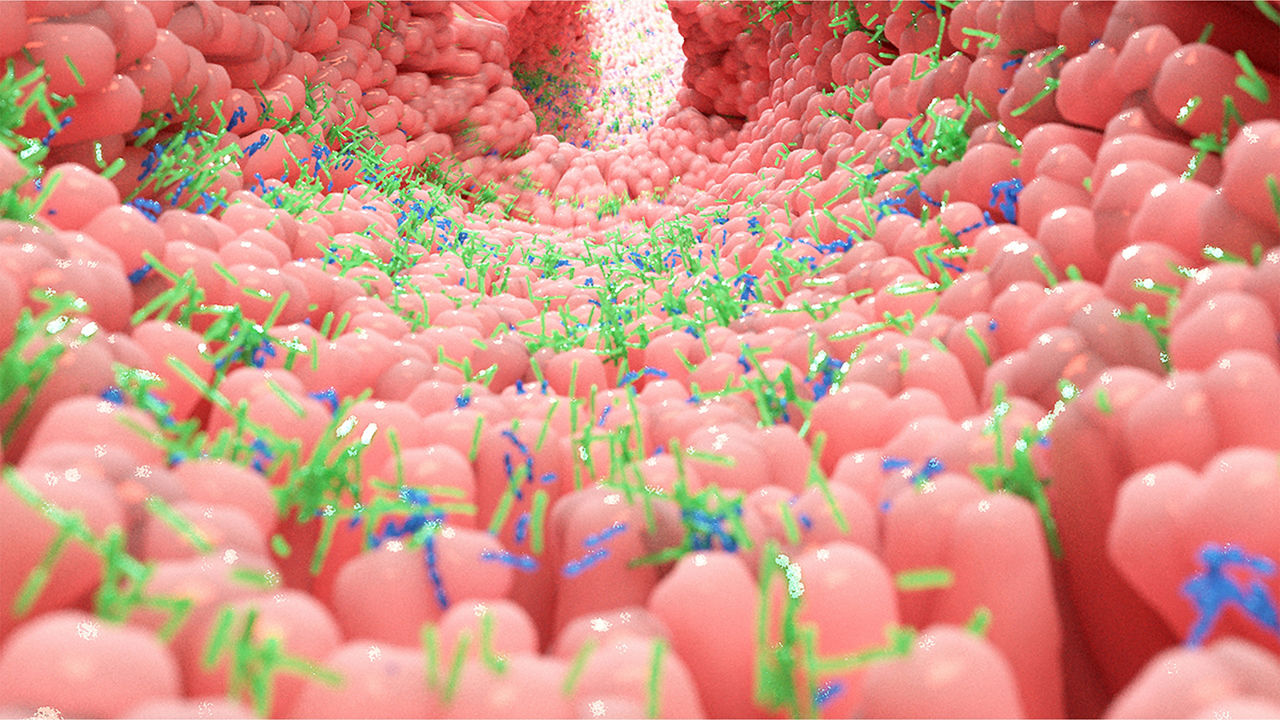
A healthy, balanced gut microbiota helps the immune system defend against pathogens, whilst tolerating otherwise harmless substances2,3, such as pollen and milk protein (leading to no or few severe allergic reactions). Conversely, an imbalanced gut microbiota – also called gut microbiota ‘dysbiosis’ – is linked to allergies and diseases such as asthma, inflammatory bowel disorders, eczema and diabetes4,5.
There is now a growing body of evidence that suggests that gut microbiota dysbiosis in early life is closely linked to the development of food allergies, including cow’s milk allergy (CMA)6,7. Compared with healthy babies, infants with CMA have an unbalanced gut microbiota with lower levels of bifidobacteria7.
Although it remains unclear exactly how gut microbiota dysbiosis leads to food allergies, studies suggest that the gut microbiota affects the immune system by changing the body’s metabolism and immune response1,4. It is possible therefore that infants with CMA, who more prone to infections8, may require not just effective resolution of their allergy symptoms but also a means of re-balancing their gut microbiota dysbiosis, which could be associated with a poorer functioning of their immune system.