EONS Education Projects - EONS - The European Oncology Nursing Society (cancernurse.eu)
Nutricia proudly sponsors EONS15 symposium on patient-centered care in nutrition
Join Nutricia at the Symposium “Person-centred interprofessional practice in nutrition – from dream to reality”
EONS15 Symposium Person-centred interprofessional practice in nutrition – from dream to reality will be held on Monday 12 September 12:00-13:30.
Learn more about the role of different health care professionals involved in the nutritional care of people with cancer. Discuss the best ways to embed clinical nutrition guidelines into clinical practice and work together to provide best care for people with cancer. Better understand the experiences of people with cancer and how we can best support to their nutritional needs.

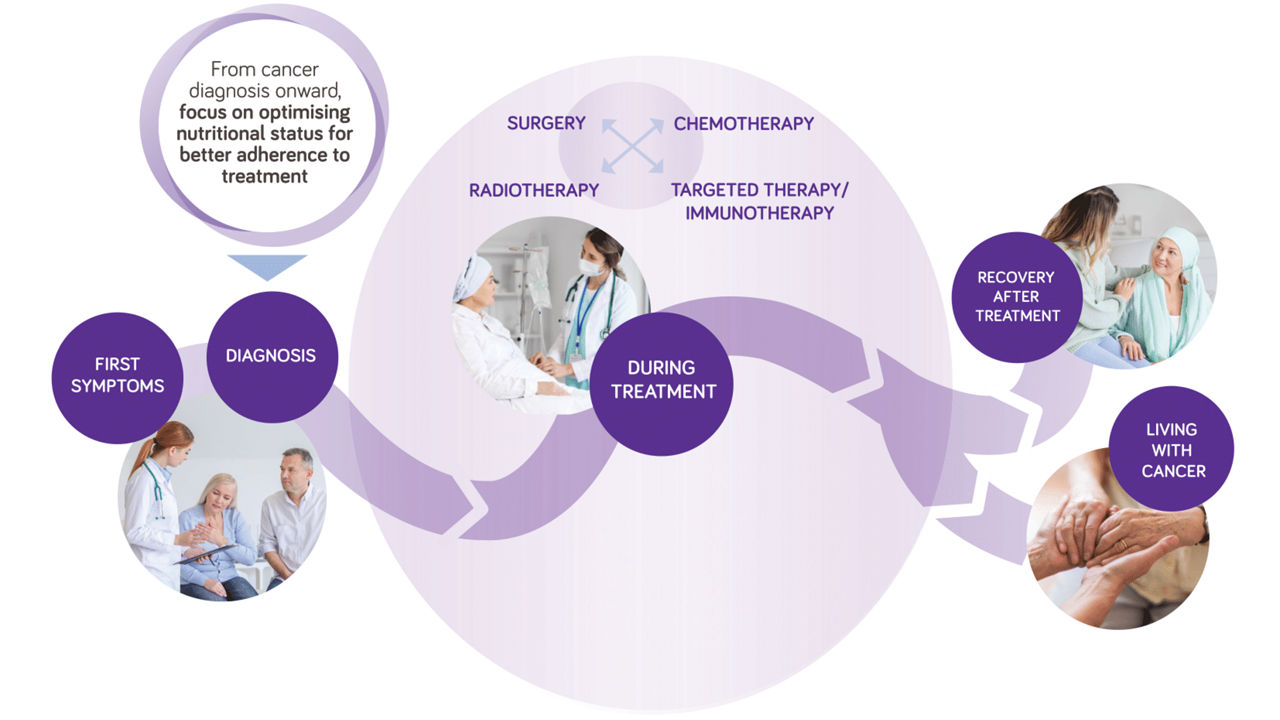
Nutritional care is important at every stop of the patient journey
Cancer treatment is a long journey. At each step, adequate nutritional status will support better treatment outcomes & quality of life1-6. Cancer treatments act a trigger of catabolism, leading to weight and muscle loss, that adversely impact clinical outcomes7-10. Early detection and treatment of malnutrition is essential to optimize cancer care11-12.
Nurses play a central role delivering patient centered care throughout the oncology treatment journey, which includes identifying nutritional risk and supporting optimal nutritional management, with medical nutrition when required.
Nurses play a key role in nutritional management
Patients with cancer frequently (30-85%) experience malnutrition and/or cachexia as a result of their disease (e.g. alterations in energy and protein metabolism), and its treatment, with side effects such as taste changes, nausea, low appetite)13-23.
Decreased food intake means that cancer patients are often deficient and/or have an inadequacy in key macro and micronutrients, which can result in significant weight loss, loss of muscle mass (cachexia) and impact physical function. Due to the negative impact of poor nutritional status on treatment tolerance and quality of life, expert and medical guidelines highlight the importance of early management of malnutrition to support patient outcomes during treatment24-31.
Cancer cachexia in adult patients
Cancer nurses have a central role in the prevention and recognition of malnutrition as well as in the management of situations that might require nutritional support:
- Follow the patients from diagnosis through to follow-up after treatment, generally spending more time with them than oncologists.
- Have an essential role in the early detection and screening of malnutrition.
- Provide necessary information and guidance to patients.
- Advise and encourage nutritional support.
- Ensure the adherence to the dietary plan32.
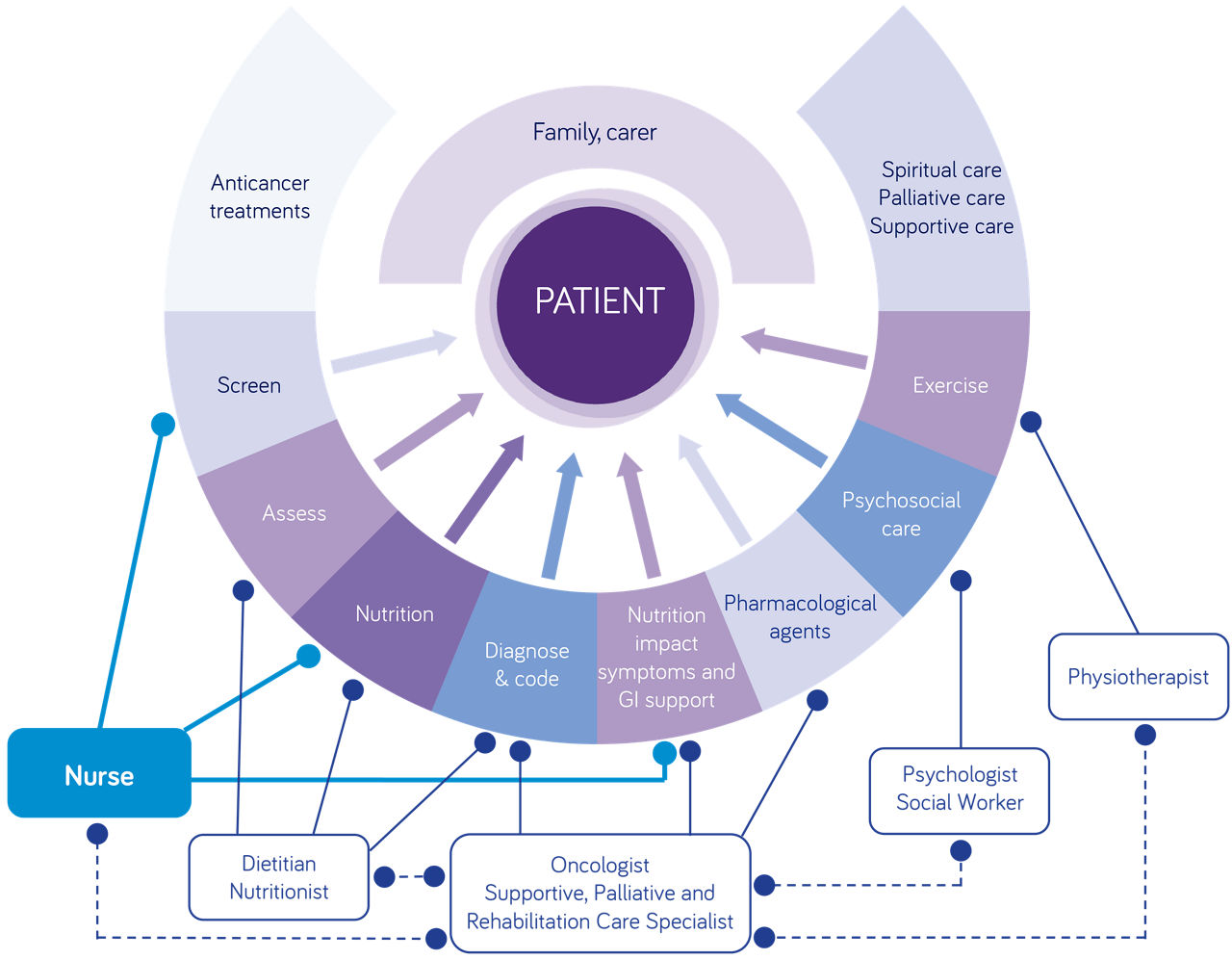
How can nurses contribute to optimal nutritional care in cancer?
The nutrition care process can be described as a few-step process, from screening and assessment of malnutrition to interventions, monitoring and evaluation. Cancer nurses are in a great position to provide support and tailored information for patients with cancer on how to manage nutrition-related challenges through whole journey.
During cancer treatment, patients may develop side effects (such as taste & smell alterations) that have a negative effect on their ability to eat. Oncology nurses can inform patients according to nutritional guidelines , provide nutritional advice , promote self-management, psychosocial support, patient education and coaching. They can , also raise and discuss nutritional issues with the oncologist and the medical team.
Nutritional screening
To facilitate early identification of nutritional issues, nurses can implement validated malnutrition screening tool that can be used at each patient visit to help identify malnutrition risk at its earliest and most treatable stage. Examples of validated tools include the Malnutrition Screening Tool, NRS-2022, amongst others. Screening is an easy step to implement before conducting nutritional assessment to define patient needs and management strategies.
Nutrition therapy should be an integrative part of cancer care. Oncology nurses have a key role to play in discuss nutritional issues and ensure they are addressed with adequate nutritional advice, nutritional interventions and referral to a dietitian or nutritionist.
Useful resources
Please find below a useful list of resources to inform nurses on nutritional management in cancer:
Please find below a useful list of resources guidelines for nutritional screening, assessment and intervention:
- Xueting et al. Clin Nutr 2021; 40;3082-3093
- Yu et al. Indian J Surg 2017; 79(1): 13–18
- Kim et al. Nutrients 2019; 11(5):1145
- Zietarska et al. Nutrients 2017; 9(10):1108
- Cereda et al. Cancer Med 2019; 8(16):6923-6932
- Grupinska et al. Nutrients 2021; 13, 3549
- Laviano et al. Proc Nutr Soc 2018; 77(4):388-393
- Ryan et al. Nutrition 2019; 67-68:110539
- Pressoir et al. Br J Cancer 2010; 102 (6), 966-71
- Daly et al. Cancer 2020; 126 (12), 2872-82
- Arends et al. Clin Nutr 2017; 6(1):11-48
- Arends et al. ESMO Open 2021; 6(3):100092
- Fearon et al. Lancet Oncol 2011; 12(5):489-95
- Arends et al. Clin Nutr, 2017; 36:1187-96
- Baracos et al. Nat Rev Dis Primers 2018; 4:17105
- Argilés et al. Nat Rev Cancer 2014; 14(11):754-62
- Vanhoutte et al. BMJ Open Gastroenterol 2016;18;3(1):e000097
- Spotten et al. Ann Oncol, 2017; 28(5):969-84
- Nejatinamini et al. Nutr Cancer, 2017; 70(3):474-82
- Nejatinamini et al. Nutrients. 2018; 10(9): 1236
- Churilla et al. BMJ Open. 2011; 1(2):e000397
- Ströhle et al. Oncology Reports 2010; 24(4):815-28
- Mardas et al. Support Care Cancer 2015; 24(6):2619-25
- Ukovic B, Porter J. Supp Care Cancer. 2020; 28(10):4575-83
- van der Schueren et al. Ann Oncol 2018; 29(5):1141-53
- Ma et al. Nutr Cancer 2016; 68(4):568-76
- Cereda et al. Radiother Oncol 2018;126(1):81-8
- Huang et al. Oral Oncol 2020; 111:105025
- van der Werf et al. Clin Nutr. 2020;39(10):3005-13
- Cox et al. Br J Cancer. 2016;115(2):172-7
- Tondulli et al. Radiother Onc. 2019;132:73
- Arends et al. ESMO Open. 2021; 6(3):100092
- Spotten et al. Ann Oncol 2017; 28:969-84
- Drareni et al. Semin Oncol 2019; 46:160-72
- Brisbois et al. J Pain Symptom Manage 2011; 41:673-83
- Boltong et al. Support Care Cancer 2012; 20:2765-74
- Belqaid et al. Acta Oncol 2014; 53:1405-12
- Prado et al. Canadian journal of dietetic practice and research 2012; 73(4):e298-303
- McCurdy et al. Nutrients 2019; 11(11)
- Stobaus et al. Nutr Cancer 2015; 67(5):818-24
- Tobberup et al. Clin Nutr ESPEN 2019; 34:94-100
- Capitao et al. Support care cancer 2022; 30(4):3007-3015
- Regueme et al. Support Care Cancer 2021; 29(2):687-696
- Hasegawa et al. Clin Nutr 2021; 40(7):4792-4798
- Kabata et al. Supportive Care in Cancer 2014; 23, 365-370
- Cereda et al. Radiother Oncol 2018; 126(1):81-88
- Grupinska et al. Nutrients 2021; 13, 3549
- Meng et al. Clin Nutr 2021; 40(1):40-46
- Manasek et al. Kin Onkol 2016; 29(5):351-357
Are you a healthcare professional or (carer of) a diagnosed patient?
The product information for this area of specialization is intended for healthcare professionals or (carers of) diagnosed patients only, as these products are for use under healthcare professional supervision.
Please click ‘Yes’ if you are a healthcare professional or (carer of) a diagnosed patient, or ‘No’ to be taken to a full list of our products.
The information on this page is intended for healthcare professionals only.
If you aren't a healthcare professional, you can visit the page with general information, by clicking 'I'm not a healthcare professional' below.




