Welcome to the healthcare professional pages of Cancer care. Here you’ll find a range of valuable information relating to the topic of cancer-related malnutrition and cachexia, including articles, clinical guidelines and products.
Cancer care
About medical nutrition
19.3 million new cancer cases in 2020[1]; malnutrition affects up to 80% cancer patients[2].
An integral part of cancer care
It is well known that cancer patients who maintain a healthy weight are likely to have better treatment outcomes3. But this can be hard thing to achieve when numerous factors can negatively affect their ability to get enough of the right nutrition. Reduced food intake due to treatment-related taste alterations and nausea, together with increased catabolic metabolism, can leave many patients malnourished and/or cachexic4-13. Medical nutrition has a clinically proven role in improving nutritional status and so helping cancer patients maintain weight14, which can give their primary treatment the best possible chance of success.

Oncology portfolio
There are health challenges adults may experience which can be managed or improved with medical nutrition (for use under healthcare professional supervision only). The Nutricia products shown from this point onwards are foods for special medical purposes and intended for the nutritional management of diseases and related medical conditions.


Discover the Nutricia Oncology Expert Day dedicated to “Taking Action to Improve Patient Care: From Guidelines to Nutritional pathways in Oncology” in Utrecht on November 25th 2024.

European Cancer Nursing Day (ECND24)
Nutricia support International Nurses Day 2024 and celebrate the role of oncology nurse during cancer care. We want to raise awareness about key role of oncology nurse within multidisciplinary team and along the continuum of cancer care.
Clinical guidelines
Congresses

Discover our educational content from Nutricia Oncology Meet the expert session
Discover our educational content from Nutricia Oncology Meet the expert session focused on ‘Optimizing oncology patient outcomes with nutritional therapy across the continuum of care’ in Madrid on October 22nd 2023.

View Educational Sessions from Nutricia’s presence at ESPEN 2023
Did you miss Nutricia at ESPEN’23? Click on the button below to learn more on the Nutricia Satellite Symposium and Educational Sessions on different topics.

Replay Nutricia EONS15 symposium on patient-centered care in nutrition
Replay Nutricia EONS15 symposium “Person-centred interprofessional practice in nutrition – from dream to reality.” Nurses play a crucial role in patient centered care in oncology, including prevention, recognition and management of nutritional challenges. Learn more about nutritional care in oncology at the EONS15 congress.
Education

Continued learning enables us all to deliver the best possible care to those who need it most. Here we bring science-led educational resources as well as news from leading medical congresses, helping to stay up-to-date with the latest advances in medical nutrition.
Patient story
Jonathan’s story
Jonathan was diagnosed with mantle cell lymphoma, one of the most aggressive forms of cancer, not once but twice. This is the story of his journey, from diagnosis, through two rounds of grueling treatments and into recovery. Jonathan is now cancer free. Watch the video and find out more about his experience, including the positive steps he took to keep his body as strong as it could be throughout, including the role of medical nutrition.
Feature articles

Taste alterations and weight loss
Sensory changes in cancer contribute to weight loss and malnutrition, increasing the risk of poor clinical outcomes15-21. Sensory-adapted oral nutritional supplements, such as the Fortimel Compact Protein Sensational flavor range, have been designed and validated with cancer patients experiencing taste and smell alterations.
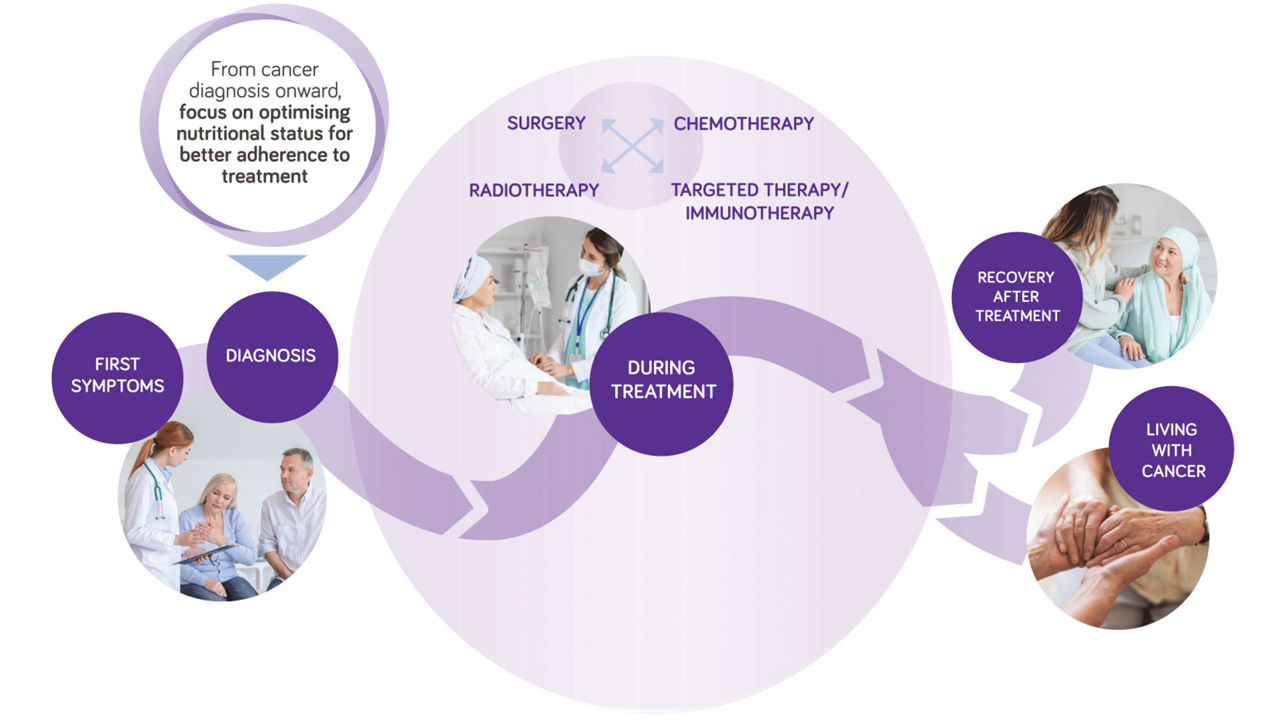
Nutritional care is important at every stop of the patient journey
Cancer treatment is a long journey. At each step, adequate nutritional status will support better treatment outcomes & quality of life1-6. Cancer treatments act a trigger of catabolism, leading to weight and muscle loss, that adversely impact clinical outcomes7-10. Early detection and treatment of malnutrition is essential to optimize cancer care11-12.
Nurses play a central role delivering patient centered care throughout the oncology treatment journey, which includes identifying nutritional risk and supporting optimal nutritional management, with medical nutrition when required.

Protein is an important nutrient at every stage of the cancer journey
Protein is an important nutrient at every stage of the cancer journey. In patients with cancer, the need for protein is higher than for healthy adults, and cancer patients often fail to consume sufficient protein33-35. Low protein intake can lead to low muscle mass, fatigue and even poorer survival in patients with cancer36-39. Therefore, ensuring sufficient protein with high protein oral nutritional supplements can improve clinical outcomes40-45.

Tastes can change, outcomes shouldn't
Up to 70% of cancer patients experience taste and smell alterations[33]. Sensory changes in cancer contribute to weight loss and malnutrition, increasing the risk of poor clinical outcomes[8,9,34-39]. Sensory-adapted oral nutritional supplements, such as the Fortimel Compact Protein Sensational flavor range, have been designed and validated with cancer patients experiencing taste and smell alterations.

ESSO collaboration
Nutricia works hard to make a positive and proven difference to patients' lives, by supporting patients, carers and societies throughout their journey with cancer and helping to deliver a better quality of life. We do so by collaborating with societies like ESSO (European Society for Surgical Oncology), to drive better nutritional support in cancer care.

Consequences of weight loss during cancer
Weight loss can affect the success of treatment22. At Danone Nutricia Research, we work with cancer specialists, academic institutions, as well as cancer patients themselves, in order to develop nutritional solutions that address patients’ needs.

Malnutrition
Cancer-related malnutrition and loss of lean body mass (‘cachexia’) are common and associated with poor outcomes for the patient. Find out more about the causes and consequences, as well as the aim of nutritional interventions at Danone Nutricia Research.
- Ferlay J, et al, eds. Global Cancer Observatory: Cancer Today. Accessed March 2022 gco.iarc.fr/today
- Laviano A, et al. Nutrition 1996;12:358-71.
- Martin L, et al. J Clin Oncol 2015;33(1):90-9
- Fearon, et al. 2011 Lancet Oncol 12(5):489-95.
- Arends, et al. 2017 Clin Nutr 36, 1187-96.
- Baracos, V, et al. Nat Rev Dis Primers. 2018;4:17105.
- Argilés JM, et al. BMJ Open Gastroenterol. 2016;18;3(1):e000097.
- Spotten et al. 2Ann Oncol. 2017;28(5):969-84.
- Nejatinamini et al. Nutr Cancer. 2017;70(3) 474-82.
- Nejatinamini et al. Nutrients. 2018;10(9): 1236.
- Churilla TM, et al. BMJ Open. 2011;1(2):e000397.
- Ströhle A, et al. Oncology Reports. 2010;24(4):815-28.
- Mardas et al. Support Care Cancer. 2015;24(6):2619-25.
- TBC
- Drareni K, et al. Semin Oncol. 2019;46:160-72.
- Brisbois TD, et al. J Pain Symptom Manage. 2011;41:673-83.
- Boltong A, et al. Support Care Cancer. 2012;20:2765-74.
- McGreevy J, et al. Support Care Cancer. 2014;22:2635-44.
- Turcott JG, et al. Nutr Cancer. 2016;68:241-9.
- Belqaid K, et al. Acta Oncol. 2014;53:1405-12.
- Bressan V, et al. Support Care Cancer. 2017;25:1699-1712.
- AS Ahmad, et al. Br J Cancer, 2015;112(5): 943–7.
Are you a healthcare professional or (carer of) a diagnosed patient?
The product information for this area of specialization is intended for healthcare professionals or (carers of) diagnosed patients only, as these products are for use under healthcare professional supervision.
Please click ‘Yes’ if you are a healthcare professional or (carer of) a diagnosed patient, or ‘No’ to be taken to a full list of our products.
The information on this page is intended for healthcare professionals only.
If you aren't a healthcare professional, you can visit the page with general information, by clicking 'I'm not a healthcare professional' below.




